When qualified plastic surgeons perform plastic surgery on the right patient in accredited facilities, desirable outcomes are likely. However, there are always risks of complications. Knowing the possibilities empowers plastic surgery patients with information useful for consultation conversations with surgeons, which leads to a better understanding of when and how to respond to complications if they occur.
In this article, we discuss possible complications that can occur with plastic surgery. We also discuss some of the risk factors and ways patients and plastic surgeons can minimize them for a happier, safer journey.
Plastic Surgery Trends
Plastic surgery is growing in popularity. According to the 2020 Plastic Surgery Statistics Report by the American Society of Plastic Surgeons (ASPS), more than 15 million cosmetic surgery procedures were performed in the United States in 2020. Social media, greater acceptance of plastic surgery, and increasing accessibility to plastic surgeons are some of the reasons patients are seeing it as a way to improve their physical appearance.

Not surprisingly, over the last three decades, plastic surgery has evolved into one of the safer surgical procedures. Advancements in plastic surgeon training, surgical techniques, strategies for patient selection, and technology have all come together to provide a satisfactory experience for most patients. Still, with any patient, there is always a risk of complications. In light of this, patients are learning more about the risks of plastic surgery and looking for ways to accomplish their physical goals safely.
Know the Risks of Plastic Surgery
Complications in plastic surgery can occur at the surgical site, or in the blood vessels, lungs, heart, and gastrointestinal (GI) system. At the surgical site, infections, hematomas, seromas, and wound dehiscence (reopening of the wound) can occur. In the blood vessels, venous thromboembolism (VTE), and fat embolism can occur leading to pulmonary embolism or death. In the GI system, surgical tools can puncture organs, or lead to infections. Within the heart, lidocaine levels and medicines like lidocaine can become toxic and cause an irregular heartbeat, which can be fatal. Lidocaine is commonly used to numb surgical areas, especially with liposuction, reducing pain and discomfort for patients. CLICK HERE to see an illustration of the possible complications of cosmetic surgery.
Infections
Infections in cosmetic surgery are rare when qualified plastic surgeons, proper patient selection, and accredited surgical facilities are the standard. According to the CDC, surgical site infections are infections that occur within 30 days of surgery. They happen when bacteria enter the open wound affecting the skin and superficial tissue. Fever, chills, and cold sweats are an indication that an infection exists. Additional signs and symptoms are pain and tenderness, redness, swelling, or warmth when touched. Patients may also notice drainage that is white, yellow, or brown with or without a foul odor. Uncomplicated surgical site infections are typically managed by antibiotics and wound care therapies.
Surgical site infections can become medical emergencies if they progress to tissue death, or move into surrounding tissues, organs, or blood vessels. Left untreated, these infections can lead to death. Patients should seek medical attention immediately if they experience any of the signs and symptoms of infection. The risk factors for surgical site infections are obesity, diabetes, immunocompromising conditions, cancer, smoking, and multiple procedures on the same day. Patients who have breast enhancements, breast reductions, and fat transfers with post-surgery drains are at greater risk for developing infections. Plastic surgeons may use antibiotic therapy during and after surgery to reduce the risk of this complication.
Hematomas
Hematomas are collections of blood that can occur near or at the site of cosmetic surgery. They happen when blood leaks out of blood vessels into tissues or under the skin. Hematomas range in size and often appear as patchy red or dark areas of the skin that can be warm, swollen, or tender. Generally, they appear within 24 to 48 hours after surgery and go away on their own as the blood reabsorbs into blood vessels. However, more serious hematomas, if left untreated, can lead to scarring, infection, or tissue death.
They are typically managed with blood pressure control, drains, compression, and other supportive therapies. A hematoma can become a medical emergency if active internal bleeding causes a significant loss in blood pressure and shock.
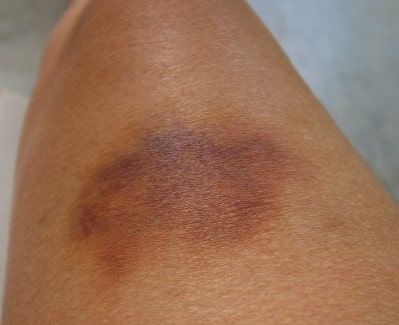
Patients and surgeons should discuss when and how to respond to hematomas that appear after surgery, especially if they notice worsening in appearance, pain, and size. Possible risk factors for hematomas are anticoagulant use, tobacco use, cancer, high blood pressure, postoperative nausea and vomiting, and BMI >30.
Seroma Risk in Plastic Surgery
A seroma is a collection of fluid in the body. It usually accumulates in an open space created by the removal of fat tissue or skin flaps during surgery. The exact reason seromas form is unknown, but they often happen after breast and abdominal surgery. To reduce seroma formation, plastic surgeons often use drains, compression garments, and surgical strategies based on their training and experience. Seromas are not life-threatening and often resolve on their own. However, if pressure is continuously applied to wounds, it can lead to the reopening of the wounds, which is called wound dehiscence. A seroma can also lead to infection if bacteria contaminate the fluid.
The signs and symptoms of seromas are long periods of swelling or drainage at the incision site after drain removal. Patients should contact their plastic surgeon if swelling with pain, tenderness, and fluid leakage increase at the surgical site beyond 7 to 10 days, or if the surgical wound begins to separate. Possible risk factors for seromas are smoking, BMI>30, breast surgery, and combined surgeries of the breast and abdomen on the same day.
Wound Dehiscence Risk in Plastic Surgery
Wound dehiscence is a separation of a wound as a result of poor wound healing, infection, or applied pressure. It usually happens 5 to 8 days after surgery and requires medical attention. If wound dehiscence results from a seroma, treatment of the seroma and the resulting wound are necessary for complete healing. Wound dehiscence is typically managed by antibiotics, the surgical removal of damaged tissues, and closure of the wound. It can become a medical emergency if left untreated leading to serious or life-threatening infection or organ exposure through the wound. Patients should talk to their surgeons about wound dehiscence, and seek medical attention immediately if a previously closed wound begins to open and show signs of infection. Some risk factors for wound dehiscence are infection, smoking, diabetes, and malnutrition.
Venous Thromboembolism Risk in Plastic Surgery
Venous thromboembolism (VTE) is the formation of a blood clot in the deep veins of the body. Deep veins are found in the lower leg, thigh, or pelvis. Certainly, they are medical emergencies when they reduce blood flow or detach from blood vessels and flow to the heart or lungs.
Pulmonary embolisms are blood clots that travel from the deep veins to the lungs, and they can be fatal. Patients should discuss VTE with their surgeons during consultations. Additionally, patients should seek medical attention immediately if they experience swelling, redness, or pain in the lower calf or legs; have shortness of breath, or have sudden chest pain.
Pulmonary embolism is a leading cause of death among plastic surgery patients. However, the risk is low when proper patient selection occurs and physicians trained in plastic surgery work in accredited outpatient facilities.
According to Rohrich & Agrawal (2020), some risk factors for venous thromboembolism include prior VTE, family history of VTE, age >40, BMI > 25, recent pregnancy, cancer, type of surgery, oral contraception use, smoking, immobility, surgery type, surgery > 6 hours, multiple procedures in the same day, and flying shortly after surgery. Some strategies for preventing deep vein thrombosis are walking to increase normal blood flow, compression, and anticoagulant therapy, for example, Lovenox (Enoxaparin).
For plastic surgeons, the prevention of venous thromboembolism is the goal. CLICK HERE to learn more about VTE.
Fat Embolism Risk in Plastic Surgery
Fat embolisms are fat particles that enter the bloodstream after fat cell and blood vessel damage. They typically occur between 2 and 3 days after surgery and can block blood flow, reduce blood-oxygen levels, and damage organs and tissues. Some signs and symptoms of fat embolisms are shortness of breath, rapid heart rate, chest pain, or fever. Patients should seek medical attention after experiencing any of these signs or symptoms. Fat embolisms can become medical emergencies if they enter the lungs and cause respiratory or heart failure, which can be fatal. Though fat embolisms are rare with trained plastic surgeons in accredited facilities, they can happen to anyone.
Highly Trained Surgeons Reduce the Risk
Ideally, patients interested in moving forward with plastic surgery should seek out plastic surgeons who completed plastic surgery residencies accredited by the Accreditation Council for Graduate Medical Education. Board certified plastic surgeons further reduce the risk of preventable complications. Board certified plastic surgeons have taken additional, optional steps to prove they have the knowledge, skills, training, and experience necessary to provide the best outcomes for patients. Plus, they must operate in accredited facilities. CLICK HERE to learn more about board certification.
Patient Selection Can Reduce the Risk
One of the best steps plastic surgeons can take to reduce the risk of complications is appropriate patient selection. In general, patients who have the greatest risks for complications:
- Have a BMI >30
- Take medications that can cause bleeding or clotting, can increase or decrease lidocaine levels in the body, or can reduce the body’s ability to fight infections
- Have a history of deep vein thrombosis (DVT) or pulmonary embolism (PE)
- Smoke cigarettes or consume nicotine products

- Have liver disease, kidney disease, uncontrolled diabetes or blood pressure, cancer, or anemia
- Have conditions that decrease the body’s ability to fight infection
- Are post-surgery or post-pregnancy
- Are receiving multiple procedures on the same day
Swelling and Bruising are Normal
After cosmetic surgery, swelling, bruising, and changes in the way skin feel are common. In fact, the process of “getting back to normal” can take between 3 to 6 months. Many patients’ journeys begin with swelling in the first 24 to 48 hours after the procedure.
This can increase over the next 10 to 14 days as the body responds to the surgery and begins the healing process. As the body heals, swelling resolves, tenderness goes away, tissues soften, and skin discoloration fades. In consultations, patients should discuss the timeline for healing and what to expect in the months post-op. Certainly, clear expectations for the months post-op increase the chances of positive outcomes at the end of the journey.
To Wrap It All Up
In the right setting, under the right conditions, plastic surgery can be a safe option for improving physical appearance. The most important elements for achieving the best outcomes are a plastic surgeon trained in a plastic surgery residency approved by the Accreditation Council for Graduate Medical Education, proper patient selection, and surgery in an accredited surgical facility. Board certified plastic surgeons can add an additional layer of safety.
As mentioned earlier, there are always risks of complications even when all of the elements mentioned above come together. Patients who are aware of the risks are able to actively discuss them with their surgeons in consultations. Additionally, knowledgeable patients are better prepared to respond to complications should they occur. Early responses to most of the complications of plastic surgery can lead to better outcomes. CLICK HERE to learn more about board certification. CLICK HERE to learn more about facility accreditation.